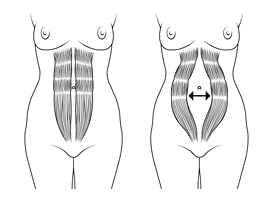
Abdominal Separation can often happen to women during or after giving birth. Most doctors say it will heal and just to continue normal daily life. We ask Osteopath, Vanessa Fisher about Abdominal Separation, the importance of helping it heal more fully and the issues with multiple births on the core stability.
Spring Fertility: Does everyone have some degree of abdominal separation during and after pregnancy?
Vanessa Fisher: Abdominal Separation or “Diastasis Recti Abdominis” – the separation of abdominal muscles – stems from what is a normal safety mechanism to avoid muscles tearing as the baby grows. Unfortunately, in what is thought to be between 50-70% of women, these muscles stay stretched and separated after the birth, causing back pain and a whole host of other issues. Theories also suggest the most susceptible to the condition are pregnant women over 35, those carrying a high weight baby or multiple babies and those in their second or subsequent pregnancies.
SF: What makes abdominal separation worse?
VF: Diastasis Recti (DR) often occurs due to the core not functioning properly, leading to misalignment, weakness and instability. Abdominal separation is a sign of excessive intra abdominal pressure. In many instances, the separation can shrink again after birth, but there can be a combination of factors during pregnancy that can cause symptoms to worsen:
– stretching the abdomen
– sit ups/crunches
– heavy lifting
– sneezing/coughing without first engaging your core
– any activity that forces the abdomen to bulge
SF:What helps it heal? Can osteopathy help?
VF: There are two ways to repair DR – abdominal surgery (a tummy tuck) or a programme including core strengthening exercises devised by your Osteopath. Most, if not all osteopaths would recommend you choose the second option, as a tummy tuck is major surgery, takes time to heal and leaves permanent scarring.
An Osteopath would devise and implement an exercise programme tailored to the patient, focusing on improvement of core stability, strengthening pelvic floor muscles and improving abdominal muscle tone. Additionally, these are some ways in which you can help your abdominal separation from worsening:
– Minimise lifting anything heavier than your baby or anything that causes your tummy to bulge with strain
– Avoid sit-ups or abdominal crunches, until the separation heals
– Roll when getting into or out of bed
– Wear an abdominal support belt or firm compressive underwear
– Implement (with specialist advice) an exercise programme to strengthen the deep abdominal muscles
SF: How long does it take to heal and do you ever get a full recovery after having abdominal separation?
VF: Every person is different, so it is impossible to put an exact timeframe on the recovery process but it is common for the separation between abdominal muscles to return to their pre-pregnancy width in 6 months to a year. A lot depends on the strength of the person’s core before the pregnancy, the size of the baby/babies, whether it’s the person’s first child and on the dedication to follow a programme of core strengthening and avoiding placing undue stress on the abdomen post-partum.
It is also worth considering that the body produces a hormone called Relaxin during and for up to six months after pregnancy. As its name suggests, this hormone allows tissues within the body to relax, meaning abdominal muscles can stretch and accommodate for an ever-growing uterus, but it also causes instability in your musculoskeletal system, leaving tissues weakened and over-stretched. Strengthening your core during and after pregnancy will not only combat the effects of carrying and delivering the baby itself, you will be fighting the negative effects of the hormone Relaxin too.
Bear in mind too that fixing or healing DR isn’t all about narrowing the gap between the rectus abdominis. Much of the online discussion around abdominal separation concentrates on the aesthetics of the “mummy tummy” and trying to return a woman to having perfect looking abdominal muscles. For many, DR leaves them with lower back pain, pelvic floor dysfunction symptoms, urinary and/or faecal incontinence or pelvic organ prolapse symptoms. Helping return a sufferer of DR to a pain-free and fully functional lifestyle, where everyday tasks can be performed well, yet with a remaining abdominal separation larger than pre-pregnancy can still be considered a success.
SF: What about multiple births – how does that affect abdominal separation?
VF: Miscarriage can be a trying and challenging time for couples. There is no ‘one way’ for navigating their path through an experience like this. In this article I have interviewed Tina Bakalla, a Demartini Facilitator, about Grief and Loss after Miscarriage to get her perspective on the issue and any useful information on how to cope.Pregnancy places the abdominals under intense stress in much the same way as a balloon expands and stretches to accommodate for enlargement. In many pregnancies, the separation of the abdominal muscles occurs and repairs without complication, but just like that balloon expanding and contracting, the more often it happens the greater the risk of instability and weakness developing.
That is not to say that a woman cannot have multiple births without DR complications. A strong core and the avoidance of heavy lifting, sit ups and crunches etc. post-birth will often mean abdominal separation occurs and heals normally after many pregnancies. The chances of DR-related issues are certainly increased, however, the more the abdominals are placed under the pressures of pregnancy.
Spring Fertility: Thanks Vanessa for sharing your insights into Recovery for our Post-Natal readers. For more information on Osteopathy to help your Abdominal Separation or Diastisis heal and recover more fully, you can contact Vanessa Fisher from The Willow Clinic on vanessa@thewillowclinic.com.au